Lifespan, Healthspan, Financialspan
In 1950, while 2.9 billion people lived worldwide, it is expected to reach 8 billion in November 2022. The average life expectancy, a general measure of population health, increased from 47 to 73 years, a 26-year increase during this time. Significant developments such as vaccination, hygiene regulations, the development of antibiotics, and early diagnosis methods that have emerged in the healthcare since the beginning of the last century, as well as the significant improvement in the quality of food and water supply, are among the main reasons for the increase in life expectancy.

Aging is known as the common cause of increase in all chronic diseases affecting millions of people today. In developed countries of the world, it is estimated that at least 25% of the population will be over 65 by 2050, and in some regions, the elderly population will exceed 40%. The increasing prevalence of elderly individuals, who are less productive and/or have chronic illnesses, also creates a heavy burden on economies worldwide.
“Despite the magnitude and certainty of the aging problem of the world population, a sufficient plan has not been developed to cope with its negative effects.”
40 million of the yearly 56 million deaths worldwide are caused by chronic diseases. According to another statistical finding, 79% of the years of disability experienced by the world population are due to chronic diseases. Respiratory diseases, cardiovascular diseases, cancers, and diabetes, which are among the top four widespread chronic diseases, are responsible for approximately 80% of deaths caused by chronic diseases. The socio-economic burden created by these diseases has been estimated to have reached approximately 47 trillion dollars in the last twenty years. 58% of deaths due to chronic diseases occur in individuals over the age of 70. Therefore, special attention needs to be given to this aging group, whose proportion in the world population is increasing day by day.
Expected increase in chronic illnesses and other conditions associated with age can result in increased care and financial burdens for families, increased pressure on public health insurance programs and authorization budgets, inadequate capacity of healthcare facilities and healthcare personnel, and negative impacts on various important aspects such as the workforce market, savings, consumption, housing, transportation, and community life.
In post-retirement life, a large majority of retirees are unable to maintain their standard of living that they used to have while actively working, let alone follow new developments and taking advantage of new opportunities. Only a very small number of retirees have a plan and opportunity to maintain the same level of comfort for 30-40 years with their savings. The lack of financial stability also plays a restrictive role in making health-related plans. Despite the magnitude and certainty of the aging problem of the world population, referred to as "Silver Tsunami" or "Gray Tsunami," a sufficient plan has not been developed to cope with its negative effects.
Lifespan refers to the total number of years lived, while Healthspan refers to the total number of healthy, disease-free years lived. When looking at the measurement of "Health Adjusted Life Expectancy (HALE)," which takes into account years lost due to disability and premature death from disease, it is estimated that there is a difference of over 9 years between Healthspan and Lifespan. It is thought that a significant portion of a person's lifespan is spent coping with illness in the last one fifth of their life cycle.
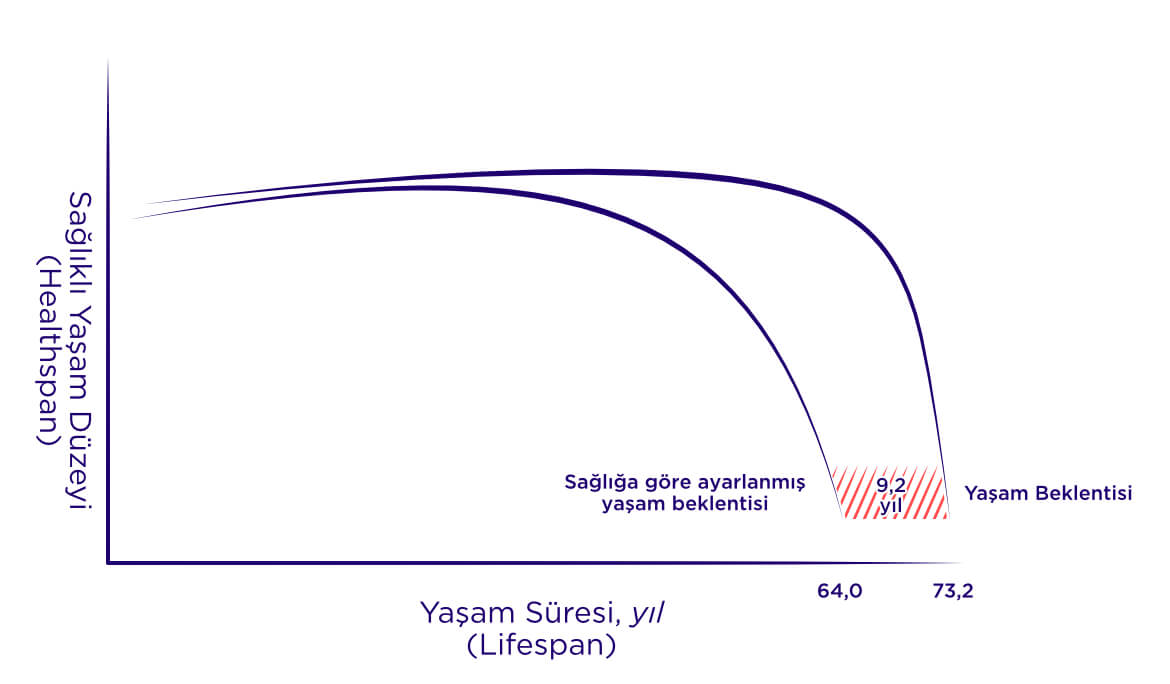
Studies on individuals with slower aging who have lived beyond 100 years old show that chronic diseases tend to begin an average of 20 years later in people who live to advanced ages. This suggests that the longevity, which focuses on extending healthy lifespan by slowing down aging, has significant potential. Calculations show the limitations of the current healthcare system, which places only partial importance on preventive medicine and focuses on managing chronic diseases and symptoms, in terms of improving overall life quality. More importantly, even if any cause of death (such as cancer, heart attack, respiratory failure, etc.) can be eliminated, this result would only extend human lifespan by a few years, as a new disease will likely emerge as a new barrier to further extending human lifespan.
The roadmap to the ideal of healthy and long life is not in preventing the diseases that arise from aging, but in the biology of aging, which is the root of these diseases. One of the most important theories in aging biology was proposed about 20 years ago by Aubrey de Grey, a biomedical gerontologist and the Scientific Affairs Director of SENS. According to de Grey, aging can be described as a three-stage process. In the first stage, as a result of metabolic processes necessary for life, various toxins are produced as an unavoidable side effect of the use of reactive chemicals. In the second, some of the damage caused by these toxins cannot be repaired by the body's endogenous repair systems and accumulates over time. In the third stage, the accumulation of damage triggers age-related pathology either by directly damaging metabolism or indirectly disrupting the repair process. According to the theory, damage accumulation can be eliminated in various ways to prevent the diseases caused by aging. As a result of this approach and subsequent scientific progress, geroprotectors have been identified in elderly people that can stop or slow down aging (such as metformin, NAD+, senolytics, rapalogs, etc.), and clinical trials for these agents have already begun.
“It is estimated that there is a difference of over 9 years between Healthspan and Lifespan.”
The personalized health sector can reach the full potential of geroprotectors by continuously monitoring biomarkers. As a result of these observations, it will be possible to avoid unnecessary and harmful drugs while selecting a special geroprotector for each patient. For example, if the inflammation level is high in a patient, regular aspirin use can extend life, while aspirin can damage tissues by inhibiting healthy inflammation processes if the inflammation level is very low, thus shortening life instead of prolonging it. Efficient geroprotector therapies can be created using artificial intelligence, machine learning, big data, and other related technologies.
Regenerative medicine involves the use of stem cells to build, renew, or improve the function of damaged organs and tissues. Backup organs and tissues can be produced outside the body using methods such as three-dimensional tissue printing. These innovations offer hope in the fight against the degenerative pathologies of aging. Another important development has been the stimulation of regeneration in the body through pharmacological means. For example, the use of prostaglandin breakdown inhibitors supports cell proliferation.
As the use of nanotechnology in medicine begins to increase, anti-aging preventatives have reached a "nano" level. Some of these preventatives contain nanoparticles such as Buckminsterfullerene (C60), which is believed to have antiviral, antioxidant, anti-amyloid, immunostimulatory and other therapeutic effects, and has been reported to increase lifespan in mice studies.
Apheresis is a procedure in which blood is taken from a patient, a specific component is removed from the collected blood, and then the blood is returned to the patient. A specialized form of this procedure, heterochronic parabiosis, has been used in recent decades in stem cell and aging research. With this procedure, the circulatory systems of one young and one elderly animal are surgically connected to each other, allowing for a single circulation system to be shared. Research results on the effect of heterochronic parabiosis on extending the lifespan of old animals have been interpreted in two ways. The shared blood source may help to reduce a factor in the old animal's blood that causes aging, or it may help the blood to enter the flow that contains a factor produced by the young animal that delays aging. If the first explanation is found to be correct, then apheresis can potentially be used to remove a factor from the blood of the elderly that causes aging.
With bionic technologies, diseased or damaged tissues, organs, or other body parts are replaced with mechanical or other artificial implants. Studies continue on artificial organs that can replace the heart, lungs, kidneys, skin, ear, eye, nose, and other organs. Advances in stem cell research, tissue engineering, and material science are giving hope for the future of artificial organs. The impact of these studies on a healthy lifespan is still unknown.
In conclusion, it is predicted that advancements in health in the coming years will result in an additional 10-20 years of life for people. In particular, stem cell research and new diagnostic technologies may make 80 feel like 60. All of these developments increase the possibility of living a long and healthy life, but also come with the need for financial management and planning. In the era where humankind will fight aging with the potential developments in the health sector, being ready for change and making long-term plans will be crucial to living a long, healthy, and active life.
References:
- Olshansky SJ. From Lifespan to Healthspan. JAMA. 2018 Oct 2;320(13):1323-1324. doi: 10.1001/jama.2018.12621. PMID: 30242384.
- Garmany A, Yamada S, Terzic A. Longevity leap: mind the healthspan gap. NPJ Regen Med. 2021 Sep 23;6(1):57. doi: 10.1038/s41536-021-00169-5. PMID: 34556664; PMCID: PMC8460831.
- Seals DR, Justice JN, LaRocca TJ. Physiological geroscience: targeting function to increase healthspan and achieve optimal longevity. J Physiol. 2016 Apr 15;594(8):2001-24. doi: 10.1113/jphysiol.2014.282665. Epub 2015 Mar 11. PMID: 25639909; PMCID: PMC4933122.
- Zealley B, de Grey AD. Strategies for engineered negligible senescence. Gerontology. 2013;59(2):183-9. doi: 10.1159/000342197. Epub 2012 Oct 1. PMID: 23037635.